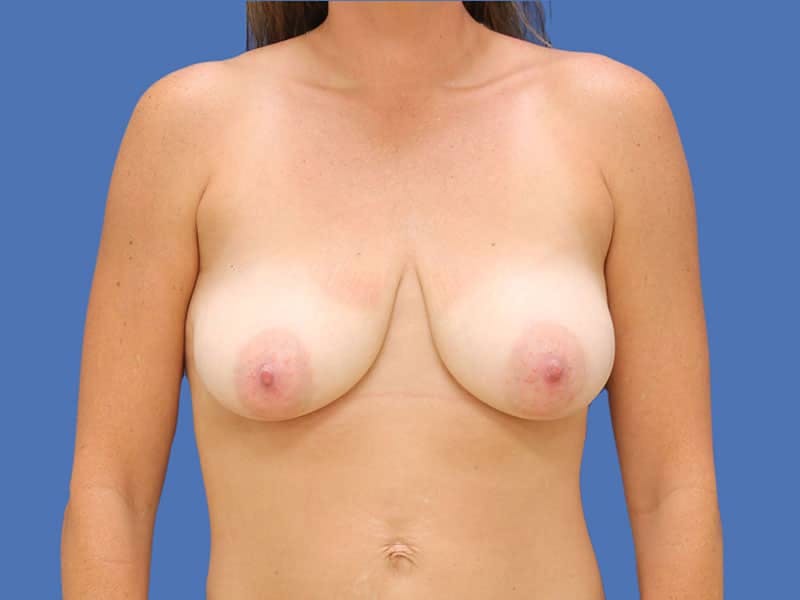
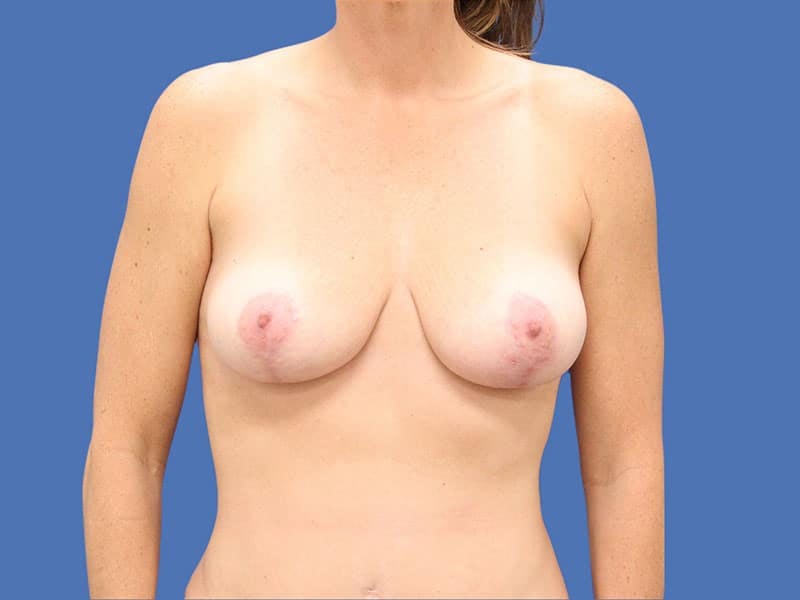
A breast lift in San Antonio at Hill Country Plastic Surgery is performed to restore the youthful lift, shape, and appearance of sagging breasts.
How is a breast lift (mastopexy) performed?
Below are the different techniques that can be used when performing a breast lift:
-
Periareolar (aka donut mastopexy): An incision is made around the areola and can be done with or without reshaping the breast tissue. Risks are nipple areolar complex (NAC) widening and pleating the tissues. This is used for patients with mild sagging who need a less extensive lift.
-
Vertical scar (also called a “lollipop mastopexy”): This incision pattern and technique is appropriate in many cases of sagging breasts. A vertical incision is made on the breast and around the areola, shaped like a lollipop.
-
Inverted T scar: This uses the traditional wise (anchor) pattern for breast reductions. This is good for severe ptosis and for patients with poor skin quality.
-
Inferior wedge excision: This technique is for patients with the proper placement of the nipple structure with extra breast tissue in the lower breast region. This incision is hidden so no visible scars are left on the breast mound itself.
- Auto-augmentation procedure: if a patient has had significant weight loss, there may be severe drooping of the breast with most of the breast tissue at the bottom. This results in what some people call a “rock in a sock” look. To create a fresh, youthful look, our surgeon will reshape the breasts, move them higher on the chest wall, and re-drape the skin over the breast to create a dramatically rejuvenated look without placing implants.